We are spending too
much on pharmaceutical products - in fact, we should be spending more.
By David J. Gibson, M.D.
Introduction
A popular perception,
belied by actual statistics, is that America is spending too much for
pharmaceutical products. On a daily basis, we are inundated with reports
of runaway costs for pharmaceuticals. Prescription drug expenditures are at an
all-time high, with retail drug costs more than doubling from 1992 to 1999,
the most current data available.
Background
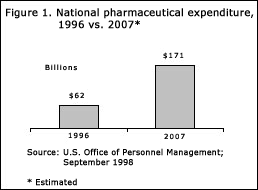
From 1992 to 1997, the number of retail prescriptions dispensed in the United States grew 23%, in 1998 by another 5% and in 1999 another 8%. Total pharmaceutical expenditures have now reached $135 billion per year. Figure 1 projects this trend over the next six years.

As a result, the pharmacy benefit within group health insurance products now
exceeds a compounded 15% annual growth rate. Current projections show that
employers will continue to face double-digit premium hikes, with prescription
drug costs serving as the biggest driver of increased costs.
Predictably, employers are restive and are now considering dropping their
pharmaceutical benefit.
As a response, HMOs have erected costly and uniformly ineffective cost
containment strategies. The HMO's prior authorization requirement
represents an expensive and labor-intensive process to manage. Many plans
quote costs of $10 to $25 per authorization request, with more than 80% of the
requests being approved. Upon review at six months, the approval
rate approaches 100%.
The role of pharmacy in health care.
In reality, providing an employer sponsored group health insurance product
without a pharmacy benefit is a shortsighted and non-viable option. Drug therapy
is now the cornerstone of modern medicine. It is the primary mode of
treatment for over 85 percent of conditions that, without therapy, would result
in the need for hospitalization of the patient.
Employers generally underestimate the costs of employee health conditions by as
much as 80% in that they overlook the effects of disability absences and lost
productivity. From this broader perspective, medical treatment costs comprise
less than 20% of what employers spend on health-related costs. Lost
productivity, or the cost of replacement staff for employees absent from work
due to short-term disability, accounted for the remaining 80% of the total cost.
In reality, strategies that optimize employee productivity through access to
adequate medical care best serve the goals of the employer in reducing overall
employee costs. Adequate medical care dictates access to pharmaceuticals.
What should we be spending?
One of the biggest problems facing the healthcare system today is patient
non-compliance with treatment. Approximately 50% of the prescriptions
written for chronic disease states are never picked up and over 66% of patients
fail to comply with their doctors' orders to take their medications.
Poor compliance is a leading cause of failed medical treatment. Even skilled
professionals often miss detecting it as the explanation for why treatment
failed. Poor compliance occurs in virtually all fields of medical care,
including organ transplant management, oral contraception, hormonal blockade to
prevent recurrent breast cancer, anti-viral treatment of AIDS,
and blinding glaucoma - fields where many assume that strong motivation would
ensure good compliance.
Patients who poorly comply substantially under-spend on prescription drugs. They
tend to delay prescription refills, are predisposed to early discontinuation of
medicines intended for life-long use, and incur costly medical complications
that could be avoided when prescribed drugs are taken correctly. Pharmaceutical
products that can reliably minimize these
problems have a substantial unrealized market potential.
The annual cost of pharmaceutical noncompliance by patients in the United States
is well documented in the literature. Noncompliance includes the
financial cost of deaths, workdays lost, hospital and nursing home admissions,
and the cost to treat the resulting adverse drug reactions. It has been
conservatively estimated that the economic costs is $100 billion or
more per year in the United States.
Conclusion
So, how much should
America allocate for pharmaceuticals within its health care system? A
conservative answer - at least twice the amount we now spend. With current
spending for pharmaceuticals in the U.S. at more than $135 billion, that
represents a current underpayment of $135 billion per year. With
compliance rates of 50% or less and the resulting cost to
treat the resulting complications exceeding $100 billion per year, this is not a
difficult proposition to advocate.
In reality, the inflationary trend for pharmaceuticals in health care represents
a primal market self-correcting force. This trend cannot be moderated by
current or yet to be conceived insurance company cost containment efforts.
Even though spending increases for pharmaceuticals in the U.S. outstrips
hospital and physician spending growth by 4 to 5 times, the role of
pharmaceuticals in the U.S. is still relatively small when compared to European
and Japanese systems.
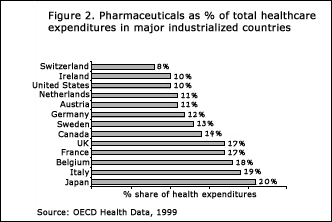
Until the U.S. health care system brings
its resource allocation into conformity with other leading industrial economies,
the inflationary trend for pharmaceuticals will continue unabated. Thus,
it is reasonable to assume that the current spending level of 10% will continue
to increase, until it reaches its natural level of 15% to 20% for overall health
care resource allocation.
The reader should consider that we are answering this question without factoring
in the new costs for genetics, biologicals, and
biopharmaceuticals that are looming upon the immediate horizon. The cost
pressures from these agents will drive the costs associated with pharmaceuticals
even higher.
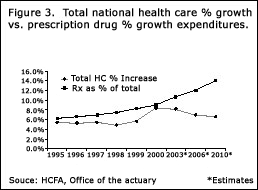
Figure 3 provides a glimpse into the future. It illustrates the predicted
percent increase in spending that we will see for pharmaceuticals vs. total
national health care spending, when projected out to the year 2010.
When viewed from the perspective of relative health care spending allocation,
two inescapable realities become apparent. The first is that America does
not need to increase its projected total health care spending. We spent $1.2
trillion (13.6 percent of the GDP) in 1999. Spending will continue to grow
through 2008, at an average rate of 6.8 percent annually,
and will reach $2.2 trillion (16.2 percent of the gross domestic product [GDP]).
The second reality is more unpleasant for health care service providers to
contemplate. Current trends dictate that we will accommodate for the growth
in spending for pharmaceuticals by decreasing the percentage of resources we
currently allocate to pay for medical services. Thus, redistributing the
current spending within health care will be used to generate the $135 in
increased pharmaceutical spending over the next few years.
© David J. Gibson, MD 2001